Treatment Methods
Various Treatments to Colon and Rectal Conditions
It is necessary to surgically remove a section or length of the colon or rectum for a variety of conditions including cancers, large benign polyps, diverticulitis, inflammatory bowel disease (Ulcerative Colitis and Crohns Disease), rectal prolapse, constipation, and for other large bowel problems that can develop. Most often a 7 to 10 inch segment of the colon or rectum is removed although in some situations a lengthier resection is carried out.
There are 2 basic methods by which trans-abdomen operations are carried; “open” and minimally invasive methods.
Up until the 1990’s the only way to carry out a colon or rectal resection was through a 5 to 9 inch long single incision in the abdominal wall that exposed the intestine. This is called the “open” approach. The most common incisions are vertical midline (up and down) and transverse (side to side). The ultimate size of the incision depends on how much colon is being resected and also on which part is being removed. Parts of the colon are mobile or “free floating” whereas others are fixed in their position. The first task for the surgeon is to mobilize the attached portions of the colon by carefully cutting the thin fibrous attachments that hold it in place. The second task is to divide and detach the blood vessels and mesentery that supply the colon segment being removed. Next, the bowel itself is divided and the specimen removed. Finally, the remaining 2 ends of the intestine are either sewn or stapled together to re-establish the continuity of the bowel. The final step is to irrigate and then close the abdominal wall incision.
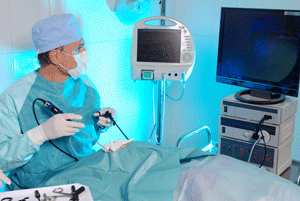
Laparoscopic Colorectal Resection (MIS)
The goal of minimally invasive colorectal surgery, which was introduced in 1991, is to minimize the trauma and injury to the abdominal wall during bowel resection. Traditionally, intestinal resections have been carried out through a lengthy incision made in the abdominal wall which provides the surgeon access to the abdominal cavity. It has been well shown that by avoiding the longer incision the patient experiences less pain and requires less pain medications. Other short term benefits include a more rapid resumption of diet, return of bowel function, and discharge home as well as the ability to walk sooner and farther than patients receiving a traditional or “open” operation. It has also been shown that laparoscopic operations cause less marked physiologic and immunologic changes than the equivalent big incision operation (see Research Section). Also, most often patients are able to return to work and full activity more rapidly. Cancer patients who require chemotherapy can also start those treatments sooner because of the faster recovery. A brief description of a laparoscopic operation follows.
After anesthesia is administered, a laparoscopic operation is begun by making a small incision (< 1 cm) near the belly button through which a hollow needle is inserted into the abdominal cavity. Carbon dioxide gas (CO2) is then pumped through the needle into the abdomen which lifts the abdominal wall off of the internal organs and creates a space in which the surgeon can work; this is called a pneumoperitoneum. A hollow tube (port) is then inserted into the abdomen through the small incision. A rigid telescope with a powerful light is then inserted into the abdomen through the port and attached to a camera which projects the image on several television monitors in the operating room. The camera provides the surgeon and his assistants with a magnified internal view of the abdominal organs. The image obtained with the high definition image systems that are used today are excellent. An additional 3 to 4 ports, with diameters ranging from a little more than a ¼ inch to ¾ inch are then placed. The ports have airtight valves on their exterior end which prevent gas leakage while allowing insertion of specially designed long surgical instruments into the abdomen. By using these instruments while watching the monitors the surgeons can work in all areas of the abdomen and can carry out the operation.
It is possible to mobilize the colon, to seal and divide blood vessels, and to divide the bowel using laparoscopic tools and without a large incision. In this way, a portion or all of the colon and rectum can be resected. Next, in order to remove the specimen it is necessary to either enlarge one of the port incisions or make a separate small incision (length is usually between 2 and 3 inches). In contrast, the standard “open” abdominal incisions usually range in size from 4 to 9 inches in length. Once the specimen has been removed, in the great majority of patients, the remaining bowel ends are rejoined and an anastomosis constructed. In some cases the rejoining of the bowel ends is done inside the abdomen laparoscopially whereas in other situations the reconnection is done externally, through the extraction incision. After completion of the anastomosis the ports and instruments are removed and the wounds carefully closed.
There are a number of different minimally invasive methods that can be used. In addition to the standard laparoscopic approach, described above, there are several other methods including; hand-assisted laparoscopic, hybrid laparoscopic/open, and the robotic laparoscopic approach. Dr. Whelan routinely uses the standard laparoscopic approach as well as the hand-assisted laparoscopic method. The latter calls for an incision large enough to accommodate the insertion of one hand into the abdomen (between 3 and 3 ½“). A special device is placed in the wound that allows the hand to be inserted yet doesn’t permit the CO2 gas in the abdomen from escaping. In this way a laparoscopic operation is carried out with one hand in the abdomen. It is then possible to palpate the bowel and to grasp and retract it which facilitates the carrying out and completion of the operation. This method is used when the segment of colon or rectum to be removed is large and bulkier than usual. It is also commonly used in obese patients in whom the standard laparoscopic operation may be more difficult. Although the final incision is usually a 2-4 cm larger than after a standard laparoscopic operation it is still at least 50% smaller than the incisions needed to do an open or big incision bowel resection.
Although at first controversial, it is now well accepted that laparoscopic colon resection is the gold standard. Laparoscopic methods have been used for almost 20 years and there are many studies and published reports attesting to the safety and presently, all parts of the colon and rectum can be removed laparoscopically; if necessary, the entire colon and rectum can be removed using minimally invasive methods. Surgeons of the Section of Colon and Rectal Surgery have done over 1,800 laparoscopic colorectal resections and have also been involved with one of the large multi-center randomized cancer trials mentioned above. In addition, Dr. Whelan has published over 85 peer reviewed publications concerning laparoscopy and the physiologic and immunologic changes associated with both laparoscopic and open bowel resection.
MIS Methods for Colon Cancer
As mentioned, during the 1990’s and up to about 2003 there was great concern and fear that laparoscopic methods might be associated with lower survival rates, higher tumor recurrence rates, and a higher rate of abdominal wall tumors. These fears led to at least 3 large randomized multicenter clinical trials which compared the traditional open (big incision) method to laparoscopic colon resection methods. Preliminary reports from these studies made it clear that there was no difference in the size of the surgical specimens removed, in the distance from the tumor to the ends of the colon specimen (called the margins), or in the number of lymph nodes removed per specimen when the open and laparoscopic pathology results were compared. Thus, it is possible to do a “radical” cancer resection laparoscopically given a skilled and experienced surgeon. Thankfully, the 3 and 5 year cancer follow up results have become available from several of these studies. The 5 year survival and local recurrence rates for the laparoscopic and open or traditional surgical methods are very similar. Also, there was no difference in the rate of abdominal wall tumors in the open and laparoscopic groups. Since the short term recovery results of the laparoscopic approach are significantly better than those of the big incision method and the long term cancer results are similar, the laparoscopic method is the surgical approach of choice.
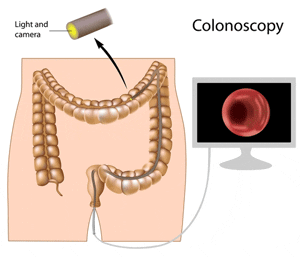
The great majority of benign colon and rectal polyps are small or moderate sized and can be removed through the colonoscope in the outpatient setting using a variety of instruments that are passed through a narrow channel in the colonoscope. Very small polyps are destroyed with a forceps that grasps and removes small pieces of the rectal lining. Larger polyps are removed most often with a metal snare (like a noose) that is passed through a thin insulated hollow plastic tube. The snare and plastic sheath are passed through a channel in the colonoscope to the scopes tip and beyond. The snare is placed around the polyp (often shaped like a mushroom) and tightened while electric current is passed through the wire. This cauterizes the stalk of the polyp while it is being cut. If possible, the polyp is recovered and sent for pathological analysis. Polyps can also be directly burned or cauterized with heat or electric current, usually after one or several biopsies have been obtained. Larger polyps, especially the flat ones, are more difficult to treat colonoscopically (See benign polyp section).
Historically, a segmental “cancer type” bowel resection is carried out to remove adenomas of the colon that are judged not amenable to removal with a colonoscope. In this case a 7 to 10 inch length of colon is resected (the polyp is usually in the middle of the specimen) along with the lymph nodes and blood vessels supplying the bowel after which the remaining ends are rejoined. Many patients ask why so much bowel is removed to treat a benign polyp? The reason is that 10 to 15 percent of large, supposedly benign, polyps that come to surgical resection are found to contain invasive cancers. Certainly, for the 10-15 percent of patients with cancers the lengthier and more extensive resection is logical and appropriate. In regards to the remaining 85-90 percent of patients with benign polyps the cancer type resection is not necessary. If there were a way to be reasonably certain that a polyp was, in fact, benign, then, perhaps, the radical resection could be avoided
An important method of judging a polyp is by taking multiple biopsies of it through the colonoscope. Another useful method is to inject saline into the bowel wall beneath the polyp to see if the polyp “lifts” off the deeper layers of the bowel wall. The injected fluid greatly expands the middle layer of the bowel wall that separates the inner lining from the outer muscle coating of the colon. If the polyp rises, then the lesion is not invading into the muscular layer (a characteristic of invasive cancers). This saline lift test is easily done through the colonoscope. Yet another method is endoscopic ultrasound which uses sound waves to determine whether the polyp is invading and into the deeper bowel wall layers. Simply taking a close look at a polyp can also provide important information to the surgeon. What are the alternatives to a full segmental cancer type resection for polyps judged benign by the above tests?
Some large benign polyps can be removed by resecting a small oval shaped piece of the bowel wall (part of the circumference only) that includes the polyp and a small rim of normal bowel wall. This is called a "wedge" resection. This operation avoids extensive dissection and does not include division of the blood vessels supplying the area or removal of the lymph nodes. In short, it is a much smaller and less radical operation that requires minimal dissection of the colon and removes far less tissue. The risk of having a complication after this type of surgery is lower because less has been done. Patients usually go home in 1 to 2 days as opposed to 3 to 5 days after the standard cancer type bowel resection.
The “wedge” resection is best performed laparoscopically. Using this method the polyp and adjacent bowel wall is resected with a narrow stapler that is inserted through a hollow 1 inch "port" in the abdominal wall. The specimen is removed through one of the laparoscopic port wounds in a plastic bag after which a pathologist immediately examines the polyp and carries out one or several "frozen sections" to verify that the lesion is an adenoma only. The patient remains on the operating room table asleep while the polyp is evaluated. In the unlikely situation that the frozen section reveals an invasive cancer, then a standard cancer type resection would be immediately carried out laparoscopically.
Another way to remove some of these polyps is to perform a colonoscopy in conjunction with laparoscopy in the operating room with the patient under general anesthesia. The laparoscopic instruments can be used to push on the outside of the colon wall to make it easier for the doctor driving the colonoscope to grasp the polyp with a snare. In this way, some polyps that could not be removed during a regular outpatient colonoscopy can be excised. It is also possible to use advanced colonoscopic polypectomy methods to remove these polyps. One such method is called ESD or Endoscopic Submucosal Dissection. In this method a thin wire connected to an electric cautery machine is passed through an insulated sheath through the colonoscope and used to make an incision around the polyp (like a knife). Then other colonoscopic tools are used to lift and dissect beneath the polyp in order to fully detach it. If successful, at the end, the polyp has been removed in one piece and the underlying muscle layer remains intact. If successful, this method avoids removing even a “wedge” of the entire bowel wall.
Dr. Whelan’s approach is to assess all patients with large benign polyps who are sent for a standard colon resection and determine if either the laparoscopic "wedge" or the combined laparoscopic / colonoscopic polypectomy methods can be utilized. The goal is to remove the polyp via the least invasive method possible. If successful, patients are home sooner with all or more of their colon in tact. Because it is not possible to be certain before surgery that a polyp can be removed via a combined laparoscopic/colonoscopic or wedge method, patients must consent to a standard colectomy in addition to the less invasive polyp removal methods. The consent states that, at the end of the procedure, the polyp will have been removed by one of the 3 methods with the standard cancer type resection being the last resort.
When the colonoscopy is performed in the operating room on the day of surgery if the polyp lifts when injected and is judged resectable via colonoscope then an attempt will be made to excise it using a variety of colonoscopic tools. If needed, the polyp can be manipulated externally with laparoscopic instruments to facilitate removal. If the polyp is successfully removed a test is done to make sure that the colon wall is not perforated after which the scopes are removed and the patient woken up.
If it is not possible to fully remove the polyp using colonoscopic methods, the borders of the polyp are marked with india ink and then an attempt is made to do a laparoscopic wedge resection of the polyp and the adjacent colon wall with a stapler. The colonoscope, still in place, views the placement of the stapler to male sure all is well. If successful, then the specimen is put in a plastic bag and removed through one of the small wounds. However, if the polyp will not lift when injected, is judged too large for colonoscopic or wedge resection, or looks like a cancer then the standard cancer type bowel resection would be immediately performed.
Pressurized intraperitoneal aerosol chemotherapy (PIPAC) is an innovative approach delivering hemotherapy into the peritoneal cavity as a pressurized normothermic aerosol. Early studies in patients with peritoneal metastases secondary to ovarian or other abdominal cancers have shown some efficacy and good tolerability, in particular PIPAC does not induce significant neither liver or renal toxicity nor gastrointestinal symptoms.
Our institution is pioneering the potential fields of the application of PIPAC, including defining indications and contraindications, chances and risks, as well as success and failures of this therapy.